Medicaid and Managed Care – Policy Brief
Medicaid and Managed Care
June 1995
This year, Medicaid will finance health and long-term care services to more than 35 million low-income Americans. In its role as a purchaser of health services for low-income families, Medicaid increasingly relies on managed care to deliver care. Almost 8 million Medicaid beneficiaries, predominately poor children and their parents, now receive health care services through a broad array of managed care arrangements, including Health Maintenance Organizations (HMOs) and less structured primary care case management systems.
Virtually every state is increasing their reliance on managed care as a health care delivery model for its Medicaid population. As of June 30, 1994, 23 percent of Medicaid beneficiaries were enrolled in managed care arrangements, up from 14 percent in 1993. Due to the growing interest in managed care from both the State and Federal governments, the number of Medicaid beneficiaries enrolled in managed care is expected to continue to rise in the foreseeable future.
This brief summarizes current trends in Medicaid managed care enrollment, describes the major models of Medicaid managed care, and raises issues for consideration with regard to managed care for low-income populations.
Medicaid Managed Care Enrollment
In response to pressures to contain the growth of State and Federal Medicaid spending and to concerns about access to health care for low-income individuals, the use of managed care arrangements in Medicaid has grown dramatically in recent years. In 1983, 750,000 beneficiaries — 3 percent of the Medicaid population — were enrolled in managed care. In 1994, about 7.8 million beneficiaries — 23 percent of all Medicaid enrollees — were enrolled in managed care arrangements. The most significant growth occurred between 1993 and 1994, when Medicaid managed care enrollment grew 63 percent, from 4.8 million beneficiaries to 7.8 million (HCFA, 1994) (Figure 1).
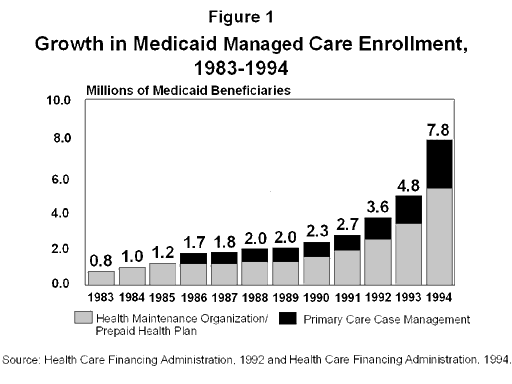
The increase in the number of managed care enrollees is paralleled by a growth in the number of states moving toward managed care for their Medicaid population. In 1981, 85 percent of all Medicaid managed care enrollment took place in four states — California, Maryland, Michigan, and New York. By 1994, these states accounted for less than a quarter (24 percent) of the Medicaid managed care population. As of June 1994, all states except for Alaska, Connecticut, Maine, Nebraska, Oklahoma, Vermont, and Wyoming reported having at least one managed care program (HCFA, 1994). Appendix Table 1 displays the number of Medicaid enrollees in managed care plans by state as of June 1994.
The growth in Medicaid managed care mirrors private sector trends. It reflects the widely held belief that managed care can improve health care access as well as promote cost containment and budget control. Changes in federal policy designed to promote the use of Medicaid managed care also have made managed care appealing to many states.
Populations Enrolled In Medicaid Managed Care
The principal populations enrolled in Medicaid managed care have been children and adults in poor single-parent families who receive Aid to Families with Dependent Children (AFDC) and low-income pregnant women and children, rather than the elderly or disabled. While low-income adults and children accounted for 73 percent of the 32.1 million Medicaid beneficiaries, their health care costs accounted for 27 percent of total program spending in 1993. Compared to the elderly and disabled, the AFDC and poverty-related populations generally require fewer and less expensive services and are, therefore, less costly.
The shift to Medicaid managed care from fee for service for the elderly and disabled population has been less dramatic. Although 18 states offered managed care plans for disabled or elderly beneficiaries eligible for Supplemental Security Income (SSI) in 1993, only a small fraction of this population is enrolled in managed care. Some Medicaid managed care programs are also directed at services for beneficiaries with specific conditions such as AIDS, high-risk pregnancy, substance abuse, mental illness, and diabetes. Two states with statewide Medicaid demonstrations, Tennessee and Oregon, include in their mandatory managed care programs acute care services for the SSI disabled and elderly populations who are not in long term care institutions.
State Options For Medicaid Managed Care Enrollment
To establish Medicaid managed care programs, a state usually must obtain one of two types of waivers from HCFA — Section 1915(b) freedom-of-choice waivers and Section 1115 research and demonstration waivers. Section 1915(b) of the Social Security Act allows states to obtain waivers to certain federal Medicaid requirements without having to meet the formal requirements of a Section 1115 program. States need this waiver to require beneficiaries to select a primary care provider and to lock them into that provider for more than one month at a time. A 1915(b) waiver is also needed for a state to operate a program in only part of the state or a program that is limited to certain categories of beneficiaries. As of October 1994, 38 states and the District of Columbia had 71 Section 1915(b) waiver programs (HCFA, 1995).
States that are interested in testing new methods of administering Medicaid and other Social Security Act programs apply for waivers of Section 1115 of the Social Security Act. Section 1115 waivers permit the Secretary of the U.S. Department of Health and Human Services (HHS) to authorize states to develop statewide managed care systems that do not meet federal statutory requirements. Up until 1993, Arizona was the only state to have a statewide Medicaid managed care demonstration. Since a liberalization and revision of the Section 1115 review and approval process in 1993, the Secretary approved statewide managed care demonstrations in eight additional states (Florida, Hawaii, Kentucky, Ohio, Oregon, Rhode Island, South Carolina, and Tennessee). Besides shifting the traditional Medicaid population into mandatory managed care, all of the recently approved section 1115 waivers extend coverage to certain low-income individuals and families not currently eligible for Medicaid. Together, the five operational statewide waivers (Arizona, Hawaii, Oregon, Rhode Island, and Tennessee) cover an estimated 1.9 million beneficiaries. (For further information, see the Commission's Discussion Brief, Medicaid Section 1115 Waivers, forthcoming)
Medicaid Managed Care Models
Generally speaking, managed care arrangements — whether under Medicaid, Medicare, or in the private sector — share certain features, including: formal enrollment by individual patients; formal contractual agreements between providers and payers; and some level of “gatekeeping” or utilization control performed either by a primary care physician or a separate administering arm of the payer, or both.
Medicaid managed care arrangements can be divided into three major types:
- Fee-for-service primary care case management (PCCM): In a PCCM, a specific provider, usually the patient's primary care physician, is responsible for acting as a “gatekeeper” — that is, approving and monitoring the provision of virtually all covered services to beneficiaries assigned to him or her. PCCM providers or “gatekeepers” contract directly with State Medicaid agencies and are paid on a fee-for-service basis. Payment generally includes a per-patient monthly case management fee to compensate for the provider's expanded administrative responsibilities. The PCCM providers do not assume financial risk for the provision of these services.
- Limited-risk Prepaid Health Plans (PHPs): Under limited risk arrangements, State Medicaid agencies contract with entities known as prepaid health plans (PHPs) to provide to enrolled beneficiaries a specified range of services. As in the case of full-risk plans, the PHP receives fixed monthly capitation payments for each eligible enrollee. The PHP often subcontracts with individual practitioners and clinics for the provision of the covered services, in the process shifting some of the financial risk to them. Additionally, some PHPs that meet the definition of an HMO are treated as PHPs through special statutory exemption.
- Full-risk plans (HMOs or HIOs): Under a fully capitated plan, State Medicaid agencies contract with a corporate entity for a fixed monthly fee per eligible enrollee for the delivery of a specified set of services. The contractor assumes the financial risk of providing all of the medically necessary services under the contract (the contractor will often reinsure against the risk of high-cost cases). The contractor often subcontracts with hospitals and other providers for the actual delivery of care, in the process shifting some of the financial risk to them. The major type of full-risk plans are Health Maintenance Organizations (HMOs), which may be Federally qualified or State certified, and in which the contracting entity and the providers are integrated into one plan. The other type of full-risk contractor is the Health Insuring Organization (HIO), which essentially operates as a fiscal intermediary and is not integrated with the provider network that actually delivers the services.
Of the 340 Medicaid managed care plans in operation in the spring of 1994, almost two-thirds were full-risk plans (HMOs or HIOs), 22 percent were limited risk PHPs, and 14 percent were PCCM arrangements. The trend among Medicaid managed care arrangements is moving away from limited-risk toward full-risk plans. As Figure 2 shows, the proportion of full-risk plans increased between 1993 and 1994 from 55 percent of total plans to 64 percent of all Medicaid managed care plans, while the proportion of PHPs declined from one third to one fifth of all plans.
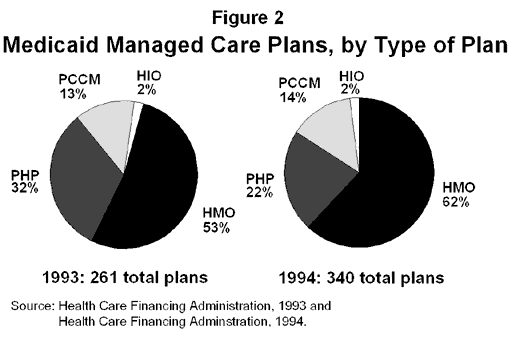
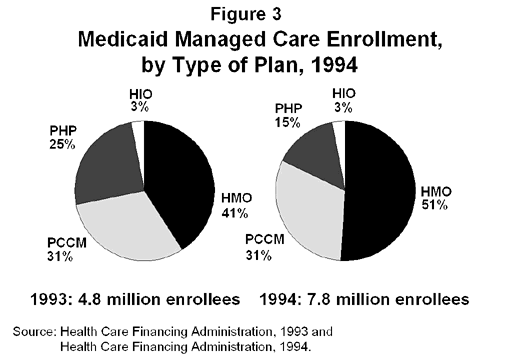
Enrollment trends mirror this trend toward full-risk contracting. Of the 7.8 million Medicaid beneficiaries enrolled in managed care as of June, 1994, more than half were enrolled in full-risk contractors(HMOs or HIOs), almost one third were enrolled in PCCMs, and less than one sixth were enrolled in PHPs. Until recently, much of the growth in Medicaid managed care enrollment came from expanded enrollment in PCCMs. However, with most of the new statewide demonstrations requiring enrollment in full-risk plans, the proportion of managed care enrollees in HMOs appears to be growing. From 1993 to 1994, Medicaid beneficiary enrollment in HMOs and HIOs jumped from 44 percent to 54 percent of all Medicaid managed care enrollees (Figure 3).
Lessons From The Medicaid Managed Care Literiture
To provide some guideposts for the use of Medicaid and managed care in the future, the Kaiser Commission on the Future of Medicaid reviewed more than 130 journal articles and studies on Medicaid's experiences with managed care to identify major findings and issues regarding access, cost, quality, and patient satisfaction. The literature reflects the diversity of approaches tried and the evolving nature of managed care. It shows that managed care is not a single model of delivering care, but rather a broad array of health care financing and delivery arrangements. The tremendous variety in the structure and scope of managed care and limitations in the study design of many of the projects make generalizations difficult. Results are often mixed across evaluations, but some common themes do emerge(Rowland and colleagues, 1995):
- Impact on access to care: There is evidence suggesting that managed care shifts the type of care and the site of care. Most studies show a decline in the use of specialist services and the use of emergency rooms as a service site. There is little evidence, however, to suggest that managed care either increases or decreases the number of physician visits, the use of preventive health services, or inpatient hospital care.
- Impact on health care costs: Evidence about cost savings are almost equally divided between studies that show program savings and those that show program costs similar to or above traditional fee for service. The literature suggests that when savings are achieved, they can range from five percent to 15 percent relative to fee for service.
- Impact on the quality of care and patient satisfaction: The quality of care in fee-for-service and managed care arrangements is about equal. Overall patient satisfaction with Medicaid and managed care is high. Satisfaction with medical care appears to be most affected by the beneficiaries' ability to remain with their previous source of care.
- Impact on special populations: Medicaid covers a wide range of low-income individuals, including families with children, the elderly, people with disabilities, and those in need of long term care. Most of the studies of Medicaid enrollees in managed care are based on low-income families and do not include elderly or disabled beneficiaries. Therefore, the experience with managed care for special populations is extremely limited.
Implications And Issues In Medicaid Managed Care
Many of managed care's principal features have the potential to improve access to care for the low-income population. By managing the beneficiary's care and ensuring that services are integrated and coordinated, managed care can overcome the fragmentation often experienced in the fee-for-service system. By promoting early intervention and preventive care, it also can lead to better access to primary care and reduced reliance on emergency rooms as a site of care. Lastly, by increasing the availability of primary care, managed care can help reduce hospitalizations for conditions that could have been treated in an ambulatory setting.
For the low-income population, realizing the potential benefits of managed care is, however, a challenging task. As the move toward managed care in Medicaid continues, a number of key issues must be addressed.
- State Implementation: Care must be taken in designing and implementing managed care systems for low-income populations. Ensuring that plans have provider networks in place, educating both providers and beneficiaries on how managed care works, and understanding the unique needs and characteristics of the Medicaid population requires a considerable amount of time and effort.
- Monitoring and Oversight: Just as overutilization is a problem in fee-for-service systems, underutilization may be a problem in managed care because care incentives are reversed. In prepaid systems where providers are reimbursed a capitated payment per individual for a range of services, there is an incentive to limit service use, particularly inpatient and specialty care. Protections and adequate enforcement, therefore, are needed to assure quality and access to health care for low-income enrollees. It also is important that payment levels to participating providers are adequate to maintain quality.
- Populations Enrolled: Medicaid covers a diverse population, that includes nine million elderly and disabled individuals. States, however, have focused their managed care expansions on children and adults in low-income families rather than the elderly and disabled populations. Due to the complex and costly health care needs of elderly and disabled populations, setting capitation rates and finding plans willing to serve this population will require considerable more effort than has occurred with managed care expansions for children and adults in low-income families. It may be prudent to use managed care demonstration programs to gain experience in developing payment rates and in recruiting an appropriate mix of specialty and primary care providers before enrolling large numbers of elderly and disabled beneficiaries into managed care programs. Unless adequate attention is given to these issues, many individuals with serious medical needs could be at risk of not getting adequate health care.
- Cost Savings: The potential for cost savings for managed care in Medicaid should be carefully evaluated. Research suggests that, in the private sector, spending on insured services would have been reduced by 17 percent nationwide if all insured people had been enrolled in group/staff model HMOs or other equally effective HMOs in 1990 (CBO, 1995). In the Medicaid program, the most rigorously designed studies suggest that managed care savings are not assured. Evidence about cost savings was almost equally divided between studies that show program savings and those that show program costs similar to or above traditional fee for service. When savings occurred, they were in the range of five percent to 15 percent (Hurley, Freund, and Paul, 1993). Several reasons will likely account for less predictable managed care savings in the Medicaid program.
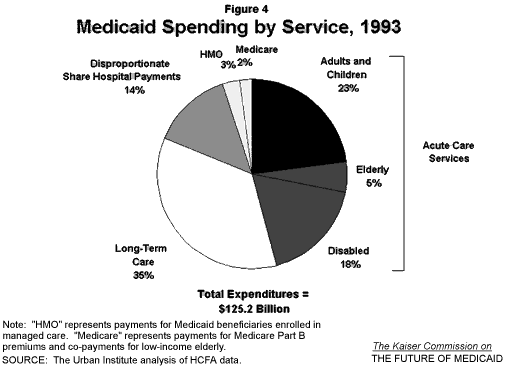
First, savings to overall Medicaid expenditures are likely to be modest because states are now primarily enrolling the least costly of the Medicaid population groups — children and adults in low-income families who primarily use acute care services. Acute care expenditures for low-income families accounted for 23 percent of total Medicaid spending in 1993 (Figure 4). Therefore, even if savings in Medicaid managed care programs are in the range of five percent to 15 percent relative to fee for service, as the literature suggests, and if all the adult and children beneficiaries were enrolled in managed care arrangements, overall Medicaid savings would amount to only one percent to two percent of total current expenditures (Holahan, 1995).
Second, operating under tight budget constraints, Medicaid has, in many cases, reimbursed providers at rates that are substantially below private sector rates. Given the low provider payment rates, savings from managed care are more difficult to achieve in Medicaid than in private health plans using discounted rates.
Finally, outreach efforts and care coordination may be more costly for a low-income population. Learning to navigate a managed care system is difficult for most health care consumers and potentially even more so for low-income individuals. Education and support services that are fairly limited in most commercial plans will be needed to provide effective health care to the low-income population.
Managed care is not an instant solution to improve access to health care for the Medicaid population and to save dollars. Making managed care work in Medicaid requires considerable attention to understanding the needs, cultural preferences, and characteristics of poor communities. Adequate time and resources in program design coupled with continuous monitoring and oversight of program implementation are needed to ensure that the potential benefits of managed care are realized.
The Kaiser Commission on the Future of Medicaid was established by the Henry J. Kaiser Family Foundation in 1991 to serve as a forum for analyzing, debating, and evaluating future directions for Medicaid reform. The Commission is not associated with the Kaiser Permanente Medical Care Program or the Kaiser Industries.
Both the Kaiser Commission on the Future of Medicaid and the Kaiser Family Foundation are involved in other analytic efforts in the area of Medicaid and managed care. The Kaiser Family Foundation, jointly with the Commonwealth Fund, is sponsoring case studies and consumer surveys in five states (California, Minnesota, New York, Oregon, and Tennessee) that are restructuring the delivery of health care to their Medicaid-eligible and uninsured populations by converting from fee for service to managed care. The Kaiser Family Foundation is also sponsoring a series of focus groups in the same states of low-income Medicaid beneficiaries concerning their experiences with, and attitudes toward, managed care.
References
Congressional Budget Office. 1995. The Effects of Managed Care and Managed Competition, CBO Memorandum, February.
Congressional Research Service. 1993. Medicaid Source Book: Background Data and Analysis (A 1993 Update), House Commerce Committee Print 103-A, January, pp. 1009-1038.
General Accounting Office. 1993. Medicaid States Turn to Managed Care to Improve Access and Control Costs, GAO/HRD-93-46, March.
Health Care Financing Administration, Medicaid Bureau. 1993. Medicaid Managed Care Enrollment Report Summary Statistics as of June 30, 1993, Washington, DC: U.S. Department of Health and Human Services.
Health Care Financing Administration, Office of Managed Care. 1994. Medicaid Managed Care Enrollment Report Summary Statistics as of June 30, 1994, Washington, DC: U.S. Department of Health and Human Services.
Holahan, John. 1995. The Implications of Past Medicaid Spending Growth for Future Debates, The Urban Institute, January.
Hurley, Robert, Freund, Deborah, and Paul, John. 1993. Managed Care in Medicaid, Ann Arbor, Michigan: Health Administration Press.
Rowland, Diane, Rosenbaum, Sara, Simon, Lois, and Chait, Elizabeth. 1995. Medicaid and Managed Care: Lessons from the Literature, Kaiser Commission on the Future of Medicaid, March.


