Using Data and Technology to Drive Process Improvement in Medicaid and CHIP: Lessons From South Carolina
In the past year, there has been a notable trend of states increasingly utilizing data and technology to modernize, streamline, and gain efficiencies in their Medicaid and CHIP programs. The expanded use of data and technology is not only helping states deal with current budget pressures and decreased administrative resources, but also lays important groundwork for the coverage expansions and new coordinated, streamlined, and technology-driven enrollment process that will go into effect in 2014 under the Affordable Care Act (ACA).
South Carolina provides a case study example of how states can utilize data and technology to improve Medicaid processes and increase enrollment for children and low-income families. In 2011, South Carolina initiated a data-driven decision making process to identify potential simplifications to its Medicaid enrollment process. This effort was in response to administrative and legislative directives to better utilize technology to reduce bureaucratic waste and improve customer service in Medicaid by eliminating unnecessary “hassle factors”. Using data analysis, the state identified significant churn in its Medicaid program—each year, about 140,000 children were losing coverage, with 90,000 returning within the year, 60,000 of whom were returning within one month. This repeated movement into and out of coverage was creating burdens for families, administrative staff, and providers.
Based on its analysis, the state determined that using eligibility information from other programs to conduct “express lane” renewals of Medicaid coverage would reduce churn and likely enable the state to earn a performance bonus. The state moved quickly to begin utilizing eligibility findings from its Supplemental Nutrition Assistance Program (SNAP) and Temporary Assistance for Needy Families (TANF) program to conduct express lane renewals and renewed coverage for about 80,000 children in just nine months. It also became one of seven states that earned performance bonuses in 2011 for the first time, earning $2.3 million of the $296.5 million awarded to a total of 23 states (Figure 1).
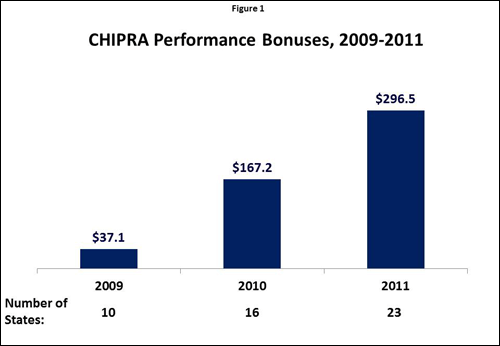
SOURCE: CHIPRA Performance Bonuses: A History (FY:2009-FY2011)
Looking ahead, South Carolina is examining how to use SNAP and TANF data to facilitate enrollment of an estimated 70,000 eligible but uninsured children into Medicaid. The state also is exploring how state staff and community partners can assure that processes move beyond enrollment to connect individuals to care. These efforts will not only increase coverage and improve care for children, but will also inform future expansion efforts under health reform by providing the state, community partners, and providers with experience enrolling large numbers of individuals at one time and connecting them to care.
South Carolina is also pursuing an update to its Medicaid eligibility system to facilitate program efficiencies and continued process improvement as well as prepare for system needs under health reform. The state is utilizing an incremental approach, focusing first on system upgrades that must be in place to meet the requirements of 2014, with additional phases planned to meet its long-term system goals. As noted, South Carolina’s efforts are reflective of the broader movement across states to increasingly utilize data and technology in their Medicaid and CHIP programs. Specifically, survey data show that as of January 2012:
- Nine states are relying on eligibility information from other income-based public programs or the state tax or revenue department to conduct express lane enrollments or renewals of children’s Medicaid or CHIP coverage. Moreover, 44 states are using an electronic data match with the Social Security Administration to verify citizenship in their Medicaid or CHIP program.
- More than two-thirds of states allow families to apply online for Medicaid and/or CHIP coverage for their children (Figure 2). Further, an increasing number of states are providing families the ability to create an online account to start, stop and return to an online application and conduct other activities such as checking benefits, reporting changes, viewing notices, or renewing coverage.
- A total of 29 states are launching major Medicaid eligibility system improvements. This significant activity has been spurred by the availability of an enhanced 90% federal matching rate (up from the regular 50% administrative federal match rate) for states to develop or upgrade existing Medicaid eligibility systems.
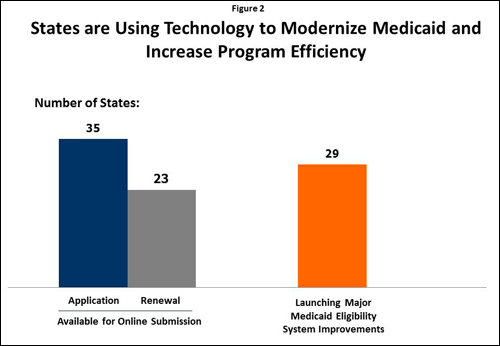
SOURCE: Based on the results of a national survey conducted by the Kaiser Commission on Medicaid and the Uninsured and the Georgetown University Center for Children and Families, 2012.
The growing use of data and technology in Medicaid and CHIP programs is leading to significant process improvements that reduce burdens for families and administrative staff and increase program efficiencies. These actions have not only helped states deal with current budget pressures, but also lay the groundwork for the 2014 coverage expansions and new enrollment requirements that are designed to provide a real-time, streamlined, technology-driven enrollment process for Medicaid, CHIP, and exchange coverage.


