Quick Take: Medicaid MCOs and Medical Loss Ratio (MLR) Requirements
One mechanism for ensuring that health insurance provides value to consumers for the premiums that they pay, or that others pay on their behalf, is to require insurers to meet a minimum “medical loss ratio” or MLR standard. The MLR is the share of premium revenues that an insurer or health plan spends on patient care and quality improvement activities, as opposed to administration and profits. In a recent 50-state survey on Medicaid managed care, conducted by the Kaiser Family Foundation’s Commission on Medicaid and the Uninsured with Health Management Associates, 11 states – Arizona, the District of Columbia, Hawaii, Illinois, Indiana, Maryland, New Jersey, New Mexico, Ohio, Virginia, and Washington – reported that they have minimum MLR requirements for their Medicaid MCOs.
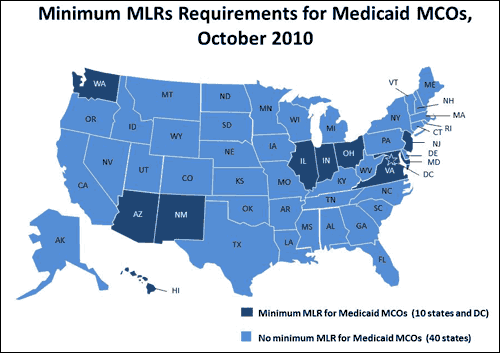
SOURCE: A Profile of Medicaid Managed Care Programs in 2010: Findings from a 50-State Survey
As explained in a related fact sheet, the Affordable Care Act (ACA) requires that, beginning in 2011, insurers in the large group market meet an MLR standard of 85% annually, and insurers in the small group and individual markets meet an MLR standard of 80%. Insurers that fail to meet these thresholds must pay rebates to their enrollees. The law permits the HHS Secretary to adjust the MLR requirement for individual coverage in a state if applying the 80% standard would destabilize the state’s individual insurance market. Seventeen states requested such MLR waivers, and the Secretary approved them for seven states (GA, IA, KY, ME, NV, NH, and NC) and rejected them for ten (DE, FL, IN, KS, LA, MI, ND, OK, TX, and WI). The ACA also requires a minimum MLR of 85% for Medicare Advantage Plans, beginning in 2014. Plans that do not meet the standard must make refunds to the HHS Secretary, and increasingly strict penalties apply for plans that fail the MLR standard more than two years in a row.
The ACA’s MLR requirements do not apply in Medicaid. This is of interest because about half of all Medicaid beneficiaries, around 27 million people, are enrolled in comprehensive, capitated managed care organizations (MCOs), and over half of these Medicaid beneficiaries are in for-profit plans. Increasingly, many states are expanding Medicaid managed care to include individuals with more complex and costly health care needs, including persons with disabilities, and “dual eligibles,” who qualify for both Medicare and Medicaid. Further, states are expected to rely heavily on MCOs to serve the 16 million additional Americans projected to gain Medicaid coverage by 2019 under the ACA.
A recent action by CMS suggests that an MLR standard in Medicaid could emerge as a federal requirement as states seek to move more and more Medicaid beneficiaries into managed care on a mandatory basis. On December 15, 2011, when CMS granted Florida an extension of its 1115 demonstration waiver, which mandates managed care for most Medicaid beneficiaries in five counties, the agency required, as one condition of the waiver extension, that MCOs in the demonstration counties meet an 85% MLR threshold beginning July 1, 2012, and provide documentation to the state and CMS to show ongoing compliance. This marks the first time CMS has ever made its approval of a state’s waiver request contingent on a minimum MLR requirement for health plans contracting with Medicaid.
The 11 states that applied MLR requirements to their Medicaid MCOs as of October 2010 reported minimum MLR thresholds ranging from 80% to 93%; most states consider direct care management a medical cost rather than an administrative one. Three states – California, Michigan, and Minnesota – indicated plans to establish an MLR requirement in Medicaid in the future. In a more recent development, Louisiana required a minimum MLR of 85% in its contracts with MCOs as the state implemented the first phase of its shift to capitated managed care in Medicaid.
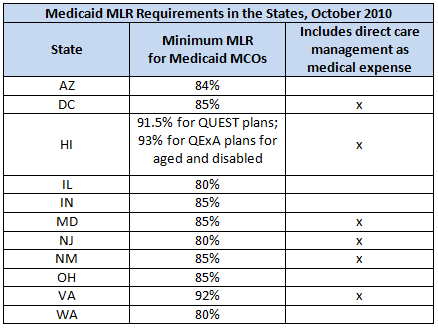
SOURCE: A Profile of Medicaid Managed Care Programs in 2010: Findings from a 50-State Survey


