Medicaid Facts: Medicaid’s Role for Children – Fact Sheet
In 1995, 17.5 million children — one-quarter of all children under age 18 — had Medicaid coverage for health care services. Medicaid, the federal/state health program for the poor, pays for a broad range of services for children including well-child care, immunizations, prescription drugs, doctor visits, and hospitalization, and a range of long-term care services for children with disabilities.
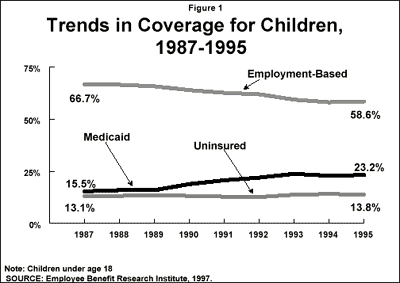
Medicaid plays a particularly strong role for low-income children, covering two-thirds (64%) of all poor children and a quarter( 27%) of children with incomes between 100% and 199% of the federal poverty level (FPL). While employer-based insurance coverage of children declined from 1987 to 1995, expansions in Medicaid have resulted in greater coverage of children in low-income families (Figure 1). During this same period, Medicaid enrollment grew from about 10 million — 15.5% of all children — to 17.5 million children (23.2%).
Despite the importance of Medicaid today, about 10 million children are uninsured. Lack of insurance is particularly high among low-income children. Seventy percent of uninsured children are in families with incomes below 200% of poverty. The new State Child Health Insurance Program, enacted as part of the Balanced Budget Act of 1997, is intended to provide coverage to this group.
Eligibility
Being poor does not automatically qualify a child for Medicaid. In the past 15 years, Medicaid eligibility for children has been broadened considerably through federal legislation and state optional expansions. Prior to 1986, Medicaid primarily served children who received AFDC cash assistance. Today, children qualify for Medicaid based on their age and income.
Medicaid coverage is especially prominent among young children, covering 33% of infants and 29% of children ages 1 to 5. Because recent expansions focused on young children, older children are less likely to qualify for Medicaid. Medicaid covers 22% of children between the ages of 6 to 12 years and 17% of teens between the ages of 13 to 18 years.
Medicaid Coverage of Children:
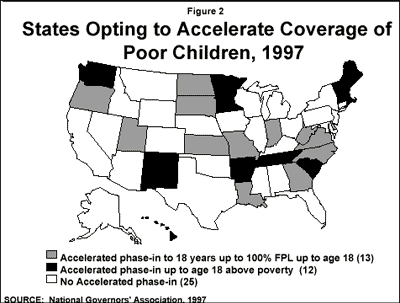
States are mandated to cover certain groups of children based on age and income criteria. By 2002, all states will be required to have phased-in coverage of children under age 19 with incomes below poverty. States can choose to expand Medicaid eligibility beyond federal minimum standards by raising age and income levels for children (Figure 2). They can also use Section 1115 research and demonstration waivers to broaden eligibility. In total, 41 states have expanded Medicaid coverage to children in one or more age or income levels. Federal coverage requirements for children are as follows:
- Up to age 6 with family incomes up to 133% FPL. For infants, 35 states have chosen to expand coverage beyond 133% FPL and 13 have expanded for children age one to six.
- Age 6 to 14 with family incomes below 100% FPL. Fifteen states have opted to expand eligibility beyond 100% FPL.
- Age 15 to 19 if family income meets the AFDC criteria of August 1996 (state average is 41% of FPL) with coverage phased-in for poor children born before 9/30/83. 25 states have opted to accelerate this phase-in to cover older children up to age 18 with income below 100% FPL (Figure 2).
- Children with disabilities also qualify for Medicaid assistance on the basis of SSI eligibility. Medicaid covers about 1 million additional children with physical or mental disabilities.
Because states established varied Medicaid income eligibility levels for children, and because of state variations in per capita income there is considerable variation in Medicaid coverage, ranging from 13% of children in Colorado to 47% in West Virginia. Similarly, Medicaid pays for 39% of all births nationally, but coverage varies from 21% of births in Massachusetts to 61% in Georgia.
The Balanced Budget Act (BBA) of 1997 creates new options for states to strengthen and expand Medicaid coverage for children. The new State Children’s Health Insurance Program (CHIP) was enacted as part of the Balanced Budget Act (BBA) of 1997. This new capped federal program allocates $20.3 billion over five years in the form of a matched grant to states to expand coverage to uninsured low-income children through either a separate state program or by broadening Medicaid — or both. The funds became available on October 1, 1997 and are targeted to uninsured children under 19 with income below 200% of poverty who are not eligible for Medicaid or not covered by private insurance.
Provisions of the Balance Budget Act also included some important changes to Medicaid. It clarifies the state Medicaid option to accelerate the phase-in for children born before September 30, 1983. In addition, the new law gives states the option to extend presumptive eligibility to children, meaning that services provided to low-income uninsured children will be covered by Medicaid before the Medicaid eligibility determination process is complete. States can also offer 12 month continuous eligibility to children, regardless of any changes in family income during that period.
Services and Costs
Federal guidelines require that Medicaid cover a comprehensive set of services with nominal or no cost-sharing for children. Access to these services is important because poor children experience more health problems than more affluent children. Children with Medicaid are eligible to receive physician and outpatient services, prescription drugs, inpatient hospital care, and long-term care services.
Medicaid coverage also entitles children to early and periodic screening, diagnostic, and treatment (EPSDT) services including a comprehensive health and developmental history and physical exam, immunizations, laboratory tests including blood lead levels, and health education. Children found to have conditions requiring further attention are covered for needed treatment.
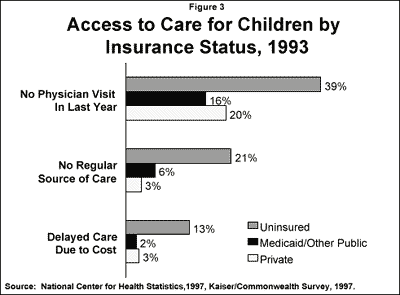
The importance of health insurance in securing access to health care services is well documented. Despite their complex health and social needs, children with Medicaid coverage have access to care that is similar to higher income privately insured children (Figure 3).
In 1995, Medicaid spent $25.4 billion on health care services for 17.5 million children in low-income families and about $7.1 billion for one million disabled children. The majority (93%) of the expenditures for non-disabled children are for acute care services, with one third for inpatient hospital care.
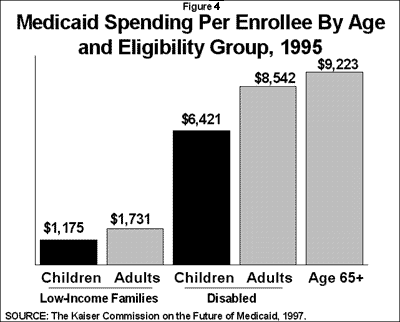
While low-income children represent half of the 35 million Medicaid beneficiaries, they account for only 16.7% of overall Medicaid spending. In 1995, Medicaid spent an average of $1,175 per low-income child enrolled in the program. On average, children cost less to care for than older Medicaid beneficiaries, but some disabled children have very costly health and long-term care needs. Medicaid spent an average of $6,421 per year per child qualifying on the basis of disability (Figure 4).
Issues and Challenges
Expanding Coverage.
To broaden coverage of low-income uninsured children, Congress enacted the new State Child Health Insurance Program and included provisions to allow states to facilitate enrollment and continuity of coverage under Medicaid. Key issues facing state Medicaid agencies include how the new children’s program will be structured, financed, and implemented, as well as how it will be integrated with or build on the state’s existing Medicaid program.
Participation.
An estimated 3 million of the 9.8 million uninsured children are eligible for but not enrolled in Medicaid. This is largely due to enrollment barriers or lack of awareness of the program. States can streamline the eligibility process and facilitate enrollment. For example, 25 states allow mail-in eligibility applications and 29 states have dropped the asset test. Medicaid eligibility policy has also changed markedly as a result of the 1996 welfare law, which eliminated the automatic link between cash assistance and Medicaid. Ongoing and intensified outreach and educational efforts will be necessary to assure that all the children who are eligible for assistance under Medicaid are enrolled.
Managed Care.
In 1996, 40% of beneficiaries were enrolled in managed care, mostly low-income children and their parents. The BBA of 1997 expands state flexibility by allowing states to mandate Medicaid managed care enrollment without requiring states to obtain a Section 1115 or 1915(b) waiver. States will still need a waiver to mandatorily enroll special needs children, but will be able to enroll other non-disabled children. Managed care has the potential to improve access to preventive and primary care, but given the vulnerable nature of the Medicaid population, it requires careful implementation and monitoring to assure quality and access.


