Pulling It Together: Rising Health Costs Are Not Just a Federal Budget Problem
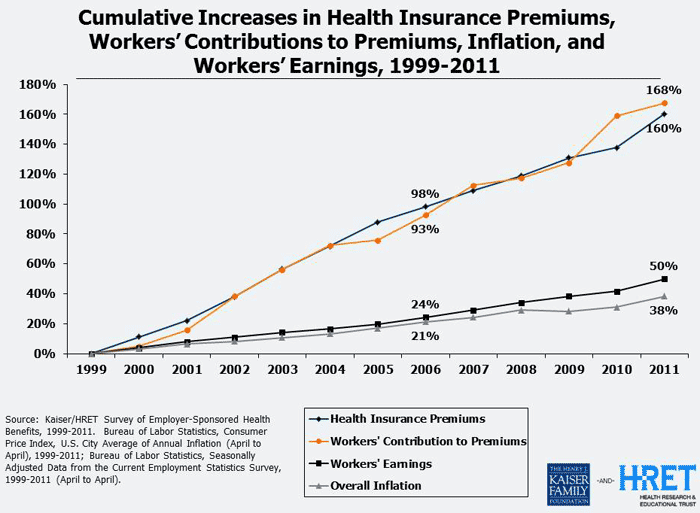
Premiums for employer-provided health insurance, where 150 million Americans get their coverage, jumped 9% in 2011 while workers’ wages grew just 2%, according to our annual employer survey. The average family policy now costs more than $15,000 per year, more than the cost of a Chevy Aveo or a Ford Fiesta. Since we began doing this survey thirteen years ago, worker contributions to premiums have increased 168%, wages 50%, and inflation 38%.
Critics of the national health reform law passed in 2010 like to blame everything but the weather on “Obamacare,” but regardless of how you feel about the Affordable Care Act, its effect on premiums this year is modest. Most of the law’s provisions don’t go into effect until 2014. The two biggest changes this year allow young adults up to age 26 to stay on their parents’ insurance policies and require some insurance plans to cover preventive services at no cost to patients. These are popular provisions that provide real benefits, and combined they account for about one to two percentage points of this year’s premium increase.
The “Supercommittee” created by the recent debt reduction legislation will be looking for more ways to save money in government health programs, but the focus in Washington is almost entirely on cutting government spending, not curbing rising health costs overall. Employers will be left to their own devices to try to keep health care costs down. They have never been very successful at this, nor have private health insurance companies. While the conventional wisdom is that private insurance does a better job of controlling costs, the opposite is true. The Centers for Medicare and Medicaid Services (CMS) says that Medicare spending per enrollee grew at a much lower rate than private insurance between 1999 and 2009 (4.9% vs. 7.2% for comparable benefits). Some say Medicare outperforms private insurance by using its purchasing power to drive a harder bargain, others, mainly providers, say it simply underpays.
In the short term, employers have few new tools to control premium increases. Employees will continue to see more high-deductible health plans, with and without tax-preferred savings accounts, and deductibles will get even larger. These plans have lower premiums because the big upfront deductible that people must pay before their insurance kicks in causes them to use fewer health services. The trend here is very clear, especially in firms with fewer than 200 employees where the percentage of workers in a plan with a deductible of $1,000 or more for single coverage has grown from 16% in 2006 to 50% today. Conservatives rail about Obamacare, but they may be winning more than they are losing; it is their vision of insurance with more “skin in the game” that is gradually taking over the marketplace because employers have no other way to control costs.
Health care groups are maneuvering with defense lobbyists and health provider groups are jockeying with beneficiary advocates about who will take the brunt of the hit from the Supercommittee. But one thing that should be clear is that reducing federal health spending is not the same thing as controlling health care costs; just ask the 150 million Americans and their employers who will be paying $15,000 when they buy a family policy this year.
