Medicare Now and in the Future
Issue
Medicare is a valuable source of health insurance for nearly 45 million Americans – mainly seniors ages 65 and older, but also 7 million younger adults with permanent disabilities. Before Medicare was signed into law in 1965, about half of all seniors lacked hospital insurance. Today, virtually all people ages 65 and over are covered by Medicare. Medicare is a popular program, but faces a number of issues and challenges in the years to come. A critical challenge is how to finance care for future generations without unduly burdening beneficiaries, taxpayers, or the general economy. Another pressing issue relates to the role of private plans in Medicare, in light of rapid enrollment growth in recent years, and concerns about the current payment system for private plans. A third issue is the relatively new Medicare prescription drug benefit and how to address concerns about its current structure and further limit the burden of prescription drug spending. Lastly, there is the challenge of how to make health and long-term care more affordable for beneficiaries in light of rising health costs.
Medicare plays a central role in broader discussions about the future of entitlement programs. Together, Medicare, Medicaid and Social Security account for more than 40 percent of the federal budget. Given ongoing concerns about the state of the economy, the candidates’ positions on these popular but fiscally challenged programs are of profound importance to the retirement security of current and future retirees.
Background
What is Medicare? Medicare plays a central role in the U.S. health care system, providing health coverage to one in seven Americans. Like Social Security, Medicare is a social insurance program that provides health coverage to individuals, without regard to their income or health status. People pay into Medicare throughout their working lives, so they and their spouses will have Medicare when they turn 65. Medicare funding comes primarily from three sources: payroll tax revenues, general revenues, and premiums paid by beneficiaries.
Who is covered by Medicare? Medicare covers a population with diverse needs and circumstances. 1
Characteristics of Medicare’s 45 Million Beneficiaries
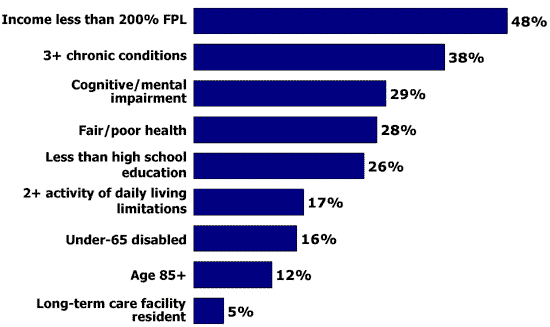
SOURCE: Current Population Survey; CMS Medicare Current Beneficiary Survey, 2006.
While many beneficiaries enjoy good health, a quarter or more have serious health problems and live with multiple chronic conditions, including cognitive impairments and functional limitations. Although the majority of the Medicare population is over age 65, 16 percent are under age 65 and permanently disabled, and while most beneficiaries live at home, 5 percent live in a long-term care setting. Many Medicare beneficiaries live on modest incomes and most depend on Social Security as their primary source of income.
What benefits does Medicare cover? Medicare provides coverage of basic health services including care in hospitals and other settings, physician services, diagnostic tests, preventive services and, as of 2006, also includes an outpatient prescription drug benefit offered through private plans. However, gaps in coverage and potentially high out-of-pocket costs are a growing concern. Medicare generally does not pay for costs associated with long-term care, which can be prohibitively expensive, nor for dental care, vision, or hearing. The traditional fee-for-service Medicare program does not have an annual cap on out-of-pocket spending and the drug benefit has a significant gap in coverage before catastrophic coverage begins.
How are Medicare benefits provided? Medicare beneficiaries have the option to get their benefits through the traditional fee-for-service (FFS) program – sometimes called Original Medicare – or through private health plans, such as health maintenance organizations (HMOs) and preferred provider organizations (PPOs) – currently called Medicare Advantage. Under traditional FFS Medicare, beneficiaries can choose to be treated by virtually any hospital or doctor, while enrolling in a Medicare Advantage plan typically requires treatment from providers in a network, or paying a higher fee to receive care from an out-of-network provider. Medicare Advantage plans generally provide all benefits covered under traditional Medicare, but many plans offer additional benefits. Today, most Medicare beneficiaries are covered under FFS Medicare, although the number of enrollees in private Medicare Advantage plans has risen dramatically in recent years, now totaling more than 10 million of Medicare’s 45 million beneficiaries. In addition, as of 2006, Medicare beneficiaries have access to subsidized prescription drug coverage offered through private plans, either stand-alone prescription drug plans, or Medicare Advantage plans.
Policy Challenges Facing Medicare
Quick Facts on Medicare Financing Challenges
- Medicare is 14% of the federal budget
- Between 2010 and 2030, the number of people on Medicare is projected to rise from 46 million to 78 million
- The Medicare Part A Hospital Insurance Fund will have insufficient funds to pay for full benefits beginning in 2019
Financing Care for Future Generations Financing care for future generations is perhaps the greatest challenge facing Medicare, due to sustained increases in health care costs, the aging of the U.S. population, and the declining ratio of workers to beneficiaries. Annual increases in health care costs are placing upward pressure on Medicare spending, as for other payers. Government experts warn that by 2019, there will be insufficient funds in the Medicare Part A (Hospital Insurance) Trust Fund to pay for benefits, 2 and most experts agree that current benefit levels cannot be sustained without additional revenue coming in to the program. Annual growth in Medicare spending is largely influenced by the same factors that affect health spending in general: increasing prices of health care services, increasing volume and utilization of services, and new technologies. In the past, provider payment reforms, such as the hospital prospective payment system, have helped to limit the growth in Medicare spending. Moving forward, system-wide efforts to curtail overall health care costs would help to improve Medicare’s financial outlook. There is general agreement among policymakers and experts that changes are needed to ensure the long-term viability of the Medicare program, but little consensus on how best to do so.
Assessing the Role of Private Plans and Providing Adequate Payments
Quick Facts on Medicare Advantage
- 10.1 million beneficiaries are now enrolled in a Medicare Advantage plan, up from 5.3 million in 2003
- Between The government pays 113% more for beneficiaries enrolled in Medicare Advantage than for beneficiaries in traditional Medicare in 2008
Since the 1970s, many Medicare beneficiaries have had the option to receive their Medicare benefits through private health plans, mainly Medicare HMOs, as an alternative to original fee-for-service Medicare. Over the past decade, Congress has made several policy changes to encourage private plan participation in Medicare and enrollment growth. A relatively generous payment system for Medicare Advantage has encouraged greater plan participation in recent years, significantly expanding the number of private plans offered throughout the country and making extra benefits available to more beneficiaries. Currently, all beneficiaries have access to at least one Medicare Advantage plan, mainly due to the emergence of new types of private plans in rural areas. 3 While some have supported the expanded role of Medicare Advantage plans as a means to improve benefits and lower costs under Medicare, the role of private plans in Medicare has been called into question in part due to the fact that the government actually pays these plans more per enrollee than if they were in traditional FFS Medicare, according to analysis by government entities.4 This payment system increases Medicare expenditures, reduces the solvency of the Part A trust fund, and increases Part B premiums paid by all beneficiaries, according to Medicare actuaries. 5
In light of Medicare’s overall fiscal challenges, many policymakers have expressed concern about the current payment system. Another concern relates to the fairness of using Medicare Advantage to provide extra benefits to enrollees, in that the majority of beneficiaries are not enrolled in Medicare Advantage plans and therefore do not receive extra benefits these plans might offer. Achieving a reasonable balance among multiple goals for the Medicare program—including keeping Medicare fiscally strong, setting adequate payments to private plans, and meeting beneficiaries’ health care needs—will be critical issues for policymakers in the near future.
Improving the Medicare Prescription Drug Benefit
After years of discussion and debate, in 2003 Congress authorized a new outpatient prescription drug benefit (Medicare Part D) that took effect in 2006. Beneficiaries can get Medicare drug coverage by enrolling in either a private plan that offers the Medicare drug benefit only or a Medicare Advantage plan that offers prescription drug coverage along with Medicare’s other benefits. The law explicitly prohibits the federal government from negotiating drug prices directly with manufacturers, pharmacies, or plans; instead, the program relies on market-based competition between private insurance plans to drive down drug costs. Since 2006, annual costs for the program have been lower than initially projected and the development of the private drug plan market has been robust, with dozens of plans available in each state. Currently nearly 26 million people on Medicare are enrolled in a Part D drug plan. 6
Quick Facts on Medicare Part D
- 90% of all Medicare beneficiaries have prescription drug coverage in 2008, but 4.6 million still have no drug coverage
- 3.4 million beneficiaries enrolled in a Part D plan had drug spending high enough to reach the coverage gap or “doughnut hole” in their plan in 2007
The experiences of Medicare beneficiaries with Part D have not been free of challenges or confusion as they confront decisions about whether to enroll in a plan and which plan to choose and learn how the benefit works. A unique feature of the benefit that is of particular concern is known as the coverage gap, or “doughnut hole”, where beneficiaries whose total drug spending exceeds a certain amount each year pay 100 percent of the costs of their drugs until they reach the level that qualifies for catastrophic coverage. The coverage gap could be a major concern for beneficiaries with multiple health conditions who may not be able to afford their medications once they reach the gap. 7
In response to ongoing concerns about certain features of the Part D program, many policymakers have called for reforms that would improve coverage or access to medications. Some would reduce or eliminate the coverage gap or “doughnut hole”, although doing so would likely result in an increase in Medicare spending which may be controversial given the fiscal challenges facing the program. Some favor changing the law to allow the federal government to use its buying power to negotiate with drug companies to try to get lower prices for prescription drugs for people on Medicare. However, proponents of the status quo are concerned that government negotiations will result in price controls that would ultimately drive U.S. drug companies to do less research and development. Another more significant change would involve the government creating its own Medicare drug plan option in which beneficiaries could choose to enroll in lieu of enrolling in a private plan.
Another issue related to Part D that continues to draw attention relates to whether people in the United States should be permitted to import lower-cost prescription drugs from other countries. Both Senator John McCain and Senator Barack Obama would allow importation of prescription drugs from other developed countries, provided the drugs are safe.
Keeping Medicare Benefits Adequate and Affordable
Quick Facts on Medicare Benefits and Affordability
- Medicare covers less than half of beneficiaries’ total medical and long-term care expenses
- Out-of-pocket spending on health care as a share of income for Medicare beneficiaries increased from 11.9% in 1997 to 15.5% in 2003 9
Despite significant protections offered by Medicare, the program is less generous than a typical large-employer plan. 8 Medicare has a relatively high deductible for inpatient care ($1,024 in 2008) and does not have a cap on out-of-pocket spending, potentially exposing people with serious medical problems to extremely high expenses. Medicare offers prescription drug coverage, but the standard benefit has a coverage gap which grows larger each year. Also Medicare does not cover long-term care expenses, which can be prohibitively expensive, nor does it pay for eyeglasses or hearing aids. As costs have risen over time, beneficiaries are spending a larger share of income on health care and premiums. 9
To help fill in Medicare’s benefit gaps and make care more affordable, many people on Medicare have some form of supplemental coverage. 10
Employer-sponsored retiree health plans are the primary source of supplemental coverage for people on Medicare, although these benefits have been eroding over time as employers grapple with rising health costs. Beneficiaries with very low incomes rely on Medicaid to supplement Medicare and Medicaid has become a critically important source of coverage for nursing home care, but beneficiaries typically have to spend down virtually all of their life savings in order to qualify for Medicaid assistance.
In the current fiscally constrained environment, there is little discussion about expanding Medicare to cover long-term care or in substantially reducing cost sharing for people covered by the program. In fact, some lawmakers have proposed changes that would reduce the growth in program spending by shifting additional costs onto beneficiaries. Examples of such policies include proposals to “means-test” benefits (that is, limit benefits only to those with low incomes), raise the age of eligibility, and increase premiums, deductibles, and cost sharing. Congress took a small step in this direction by charging higher Part B premiums for Medicare beneficiaries with higher incomes (over $82,000/single; $164,000/couple in 2008). A similar proposal would subject more beneficiaries to higher premiums for their Medicare Part D coverage.
Assessing Candidate Positions
Medicare has not emerged as a central issue in 2008 and neither of the presidential campaigns or major political parties has released a detailed set of Medicare policy proposals or specific measures to achieve long-term fiscal balance. Discussion of Medicare policy to date has focused generally on the role of private plans in Medicare, ways to lower the cost of prescription drugs, and system-wide changes to reduce health care costs overall, such as adopting electronic medical records, increasing preventive care, and improving chronic care delivery. However, the direction and pace of reform will be significantly affected by the election outcome. The future direction of the program appears to be governed by differences in ideology, particularly the role of government versus the role of the private sector. The broad visions of how Medicare should be designed in the future and how Medicare benefits should be provided will inform the policy choices made by Congress and the administration over the next four years. Therefore it is important to carefully consider the policy recommendations of the candidates to understand their vision for the future of Medicare.
The following questions are intended to help discern the candidates’ approaches to Medicare reform.
QUESTIONS FOR THE CANDIDATES
- What specific strategies would you recommend to keep Medicare financially secure for future generations?
- Would you support means-testing Medicare, limiting benefits only to those with low incomes?
- Do you think higher-income people on Medicare should be asked to pay more than others for their Medicare benefits? How would you define “higher income?”
- Would you support charging higher premiums to those with higher incomes for the Medicare drug benefit, as for Part B (physician services)?
- What is the appropriate role of private health plans in Medicare? Do you support the current payment system for Medicare Advantage plans?
- How would you propose to improve the Medicare drug benefit? Do you support eliminating the coverage gap, allowing the government to negotiate drug prices, or allowing beneficiaries to import drugs from abroad? How would you pay to eliminate the coverage gap?
- How would you propose to help people on Medicare and their families with the rising cost of medical care and the high cost of long-term care?
1 Data for this section come from Kaiser Family Foundation analysis of the Centers for Medicare and Medicaid Services Medicare Current Beneficiary Survey.
2 2008 Annual Report of the Boards of Trustees of the Federal Hospital Insurance and Federal Supplementary Medical Insurance Trust Funds.
3 M. Gold, “Medicare Advantage in 2008”, Prepared for the Kaiser Family Foundation, June 2008; available at http://www.kff.org/medicare/7775.cfm.
4 Medicare Payment Advisory Commission analysis of plan bid data from CMS, November 2007.
5 2008 Annual Report of the Boards of Trustees of the Federal Hospital Insurance and Federal Supplementary Medical Insurance Trust Funds.
6 Centers for Medicare and Medicaid Services, Medicare Advantage, Cost, PACE, Demo, and Prescription Drug Plan Contract Report – Monthly Summary Report, September 2008.
7 J. Hoadley, E. Hargrave, J. Cubanski, and T. Neuman, “The Medicare Part D Coverage Gap: Costs and Consequences in 2007,” Kaiser Family Foundation, August 2008; available athttp://www.kff.org/medicare/7811.cfm.
8 D. Yamamoto, T. Neuman and M. Strollo, “How Does the Benefit Value of Medicare Compare to the Benefit Value of Typical Large Employer Plans?” Kaiser Family Foundation, September 2008; available at http://www.kff.org/medicare/7768.cfm.
9 P. Neuman, J. Cubanski, K. Desmond, T. Rice, “How Much ‘Skin In The Game’ Do Medicare Beneficiaries Have? The Increasing Financial Burden of Health Care Spending, 1997-2003” Health Affairs, November/December 2007; available at http://www.kff.org/medicare/med110107oth.cfm; K. Desmond, T. Rice, J. Cubanski, P. Neuman, “The Burden of Out-of-Pocket Health Spending Among Older Versus Younger Adults: Analysis from the Consumer Expenditure Survey, 1998-2003”, Kaiser Family Foundation, September 2007; available at http://www.kff.org/medicare/7686.cfm.
10 Kaiser Family Foundation, “Examining Sources of Coverage Among Medicare Beneficiaries: Supplemental Insurance, Medicare Advantage, and Prescription Drug Coverage — Findings from the Medicare Current Beneficiary Survey,” August 2008; available at http://www.kff.org/medicare/7801.cfm.