Quick Take: An Update on the ACA & HIV: Medicaid Health Homes
We recently wrote about the different ways in which the Affordable Care Act (ACA) changes pathways to health insurance coverage for people with HIV, and chronicled these specifics, as well as several outstanding questions, in a policy brief. As we noted, among the many provisions of the ACA designed to improve care is a new option available to state Medicaid programs to provide “health homes” for Medicaid enrollees with chronic conditions, with a temporary enhanced federal match of 90%. The law specified several chronic conditions that could be targeted by the health home model but did not include HIV. However, the law also authorized the Secretary of Health and Human Services to expand the list, and HHS guidance issued to states in November 2010 signaled that such an addition might be considered. Moreover, HHS has already approved this option for two states that sought permission to include people with HIV in their Medicaid health home models. On November 29, 2012, the Secretary announced that HIV will formally be added to the list of chronic conditions (with a new rule forthcoming), in a move that is seen as signal to states about the importance of considering this population in the health home model in their Medicaid programs.
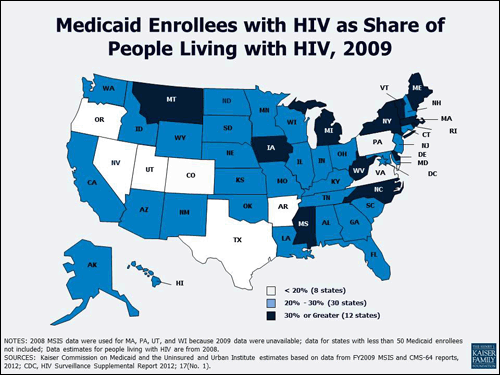
Medicaid, the nation’s principal safety-net health insurance program for low-income Americans, is a critical source of care and coverage for people with HIV, providing them with a range of needed services including antiretrovirals and other prescription drugs. Medicaid is estimated to cover half of people with HIV in regular care and about a quarter of those who have been diagnosed. In 12 states, Medicaid covers 30% or more of the state’s HIV population (see Figure).
Why are health homes important for HIV care and prevention?The idea of a health home is to provide “person-centered”, or “whole-person” care to those with chronic conditions. It has its roots in the longer history of the patient-centered medical home (PCMH) model, and emphasizes the importance of providing medical homes as a way to engage patients and coordinate care to achieve better health outcomes, lower costs, and enhanced quality. The health home has also been an important part of HIV care over the course of the HIV epidemic – and thus far has been a main by-product, and key feature, of the Ryan White HIV/AIDS program, the nation’s federal grant program for uninsured and underinsured people with HIV. What makes the Medicaid health home option significant is it that it provides a platform for adapting successes from Ryan White’s flexible grant funding model to an insurance model, which has historically been much more focused on paying for discrete medical care services.
Today, the HIV “health home” is perhaps even more critical, given that antiretroviral treatment not only provides tremendous health benefits to patients with HIV, but also, recent research has found significantly reduces the risk of transmitting HIV. Yet, data indicate that most people with HIV in the U.S. are falling off the “treatment cascade” – the continuum between HIV diagnosis and viral suppression – with the biggest cliffs occurring between linkage to and retention in care. This demonstrates that people with HIV often need more than primary care and a prescription drug benefit to remain engaged in care. And this is the very type of challenge the health home model is designed to address.
Why a health home in Medicaid? Many individuals served by Medicaid have complex and chronic health care needs. Under the ACA, these beneficiaries are potentially eligible for health home services if they have at least two chronic conditions, have one chronic condition and are at risk for another, or have one serious and persistent mental health condition. The chronic conditions specified in the law were mental health, substance use, asthma, diabetes, heart disease, and being overweight and, as mentioned above, the law authorized the Secretary to expand the list.
While the health home option is important for Medicaid enrollees overall, since many have two or more chronic conditions, it is particularly important for Medicaid enrollees with HIV. Not only are most enrollees with HIV disabled (74%), half are dually or triply diagnosed with mental illness and/or substance use – more than twice the rate among enrollees without the disease (22%) – and Medicaid spending on those who are dually and triply diagnosed is also very high.
States that take up this option for their current enrollees with chronic conditions, as specified in their approved models, will also serve new enrollees in the population they target, including the many low-income, uninsured adults expected to come onto the program in 2014, when the ACA’s new Medicaid eligibility rules take effect (see: http://www.kff.org/healthreform/8348.cfm).
Medicaid health home services and HIV care?Under the ACA, health home services encompass a range of services designed to help manage care for those who are chronically ill:
- comprehensive care management;
- care coordination and health promotion;
- comprehensive transitional care from inpatient to other settings, including appropriate follow-up;
- patient and family support;
- referral to community and social support services; and
- use of health information technology (HIT) to link services.
Of note, these are the very types of services recommended for engaging and retaining people with HIV in care, needed to produce good clinical outcomes and manage costs. To date, however, Medicaid programs have often had limited coverage of these services. This has meant that the Ryan White program, which receives capped funding each year that has never been sufficient to meet all needs, must fill in for these gaps within Medicaid. With the health home option, these services can be paid for by Medicaid – states will receive an enhanced federal match of 90% for these services for two years, and thereafter their regular Medicaid match.
Medicaid health home providers and HIV providers?The ACA specifies the types of providers that can qualify as health homes:
- Designated provider: A physician, clinical/group practice, rural health clinic, community health center, community mental health center, home health agency, pediatrician, OB/GYN, or any other provider determined appropriate by the state that meets qualification standards to be set by the Secretary.
- Team of health professionals operating with a designated provider: May include physicians and other professionals, such as a nurse care coordinator, nutritionist, social worker, behavioral health professional, or any professionals deemed appropriate by the state.
- Health team: The team may include medical specialists, nurses, pharmacists, nutritionists, dieticians, social workers, behavioral and mental health providers, chiropractors, licensed complementary and alternative medicine practitioners, and physicians’ assistants.
These definitions are broad, and could include providers with HIV expertise, including Ryan White providers, if states sought to designate them as part of their health home team model.
What is next?To date, seven states have already received approval to provide Medicaid health homes, another seven have submitted proposals to CMS for health homes, and several others have planning grants to help develop their models. Two states with approval – New York and Oregon – sought and received permission to include people with HIV in their target populations and one with a proposal under review – Alabama – also proposes to include people with HIV. The new rule explicitly including people with HIV is expected to send a signal to states about the importance of considering the health home option for this population.
While stakeholders in the HIV community await the new rule from HHS, there are several issues and questions to consider going forward:
- To what extent will the new rule address the need for states to include experienced HIV providers, including Ryan White providers, in their HIV health home teams? Given historic challenges of coordination between state Medicaid and health departments, how will linkages be addressed? This question has bearing on the ACA’s broader Medicaid expansion provisions, where new provider networks will need to be formed and the HIV community has expressed concern about the inclusion of Ryan White providers.
- Are there specific lessons to be learned from New York and Oregon about their experiences to date? How have they included HIV providers in their health home teams for people with HIV? What specific efforts were made to engage and retain people with HIV in care?
- How will other states learn about the availability of this new option, particularly those with significant numbers of Medicaid enrollees with HIV?; and
- Ultimately, how will the health home model contribute to both the public health and clinical promise of HIV treatment in those states that adopt it, helping to reduce the size of the “cliffs” along the HIV treatment cascade?