Eliminating Racial/Ethnic Disparities in Health Care: What are the Options?
Racial and ethnic disparities in health care – whether in insurance coverage, access, or quality of care – are one of many factors producing inequalities in health status in the United States.1 Eliminating these disparities is politically sensitive and challenging in part because their causes are intertwined with a contentious history of race relations in America. Nonetheless, assuring greater equity and accountability of the health care system is important to a growing constituency base, including health plan purchasers, payers, and providers of care. To the extent that inequities in the health care system result in lost productivity or use of services at a later stage of illness, there are health and social costs that affect us all.
Why Health Care Disparities Are a Concern
One in three residents of the United States self-identify as either African American, American Indian/Alaska Native, Asian, Native Hawaiian/Pacific Islander, Hispanic/Latino, or multiracial. By 2050, this number is expected to increase to one in two.2
Despite significant advances in civil rights, race remains a significant factor in determining whether an individual receives care, whether an individual receives high quality care, and in determining health outcomes.
The Institute of Medicine (IOM) landmark report, Unequal Treatment, provides compelling evidence that racial/ethnic disparities persist in medical care for a number of health conditions and services.3 Numerous efforts are underway to reduce or eliminate racial and ethnic health care disparities, and to address some of the social factors that affect health care outcomes. Yet despite these many efforts, disparities in access to quality care remain, and for some measures being tracked, gaps in care are getting larger rather than smaller.4
Key Facts on Race, Ethnicity and Health Care in the U.S.
Racial/ethnic disparities in health persist today even when comparing groups of similar SES. For example, the infant mortality rate for college educated Black women is higher than that for White women with similar education (11.5 vs. 4.2 per 1,000 live births).
The rate of new AIDS cases in 2003 was 3 times higher among Hispanics and 10 times higher among African Americans than among Whites (26 and 75 per 100,000 vs. 7 per 100,000).
At least 1 in 3 nonelderly Latinos (36%) and AI/ANs (33%) is uninsured, as compared with 22% of African Americans, 17% of Asian and Pacific Islanders, and 13% of Whites.
Insurance matters, as evidence by the fact that uninsured adults across racial/ethnic groups are at least twice as likely to go without a doctor visit in the past year.
Black and Latino adults are less likely to rely on a private physician for their medical care than White adults (62% and 44% vs. 77%).
African American children have a rate of hospitalization for asthma that is 4 to 5 times higher than the rate for White children (527 per 100,000 vs. 144 per 100,000).
Disparities in quality of care are not getting smaller. Over time, the gap between Whites and African Americans, Hispanics, Asians, and AI/ANs has either remained the same or worsened for more than half of the core quality measures being tracked.
ADDRESSING HEALTH CARE DISPARITIES
Although attention to racial/ethnic disparities in care has increased among policymakers, there is little consensus on what can or should be done to reduce these disparities. The U.S. Congress provided early leadership on the issue by legislatively mandating the IOM study on health care disparities, creating the National Center on Minority Health and Health Disparities at the National Institutes of Health, and requiring DHHS to produce the National Healthcare Disparities Report.5 This brief examines four broad policy areas for addressing racial and ethnic health care disparities:
- Raising public and provider awareness of racial/ethnic disparities in care;
- Expanding health insurance coverage;
- Improving the capacity and number of providers in underserved communities; and
- Increasing the knowledge base on causes and interventions to reduce disparities.
Raising Public and Provider Awareness
Perceptions of a problem often influence the actions taken (or not taken) to change policy and practices. If the public or providers are unaware that a problem exists, or misunderstands the nature of the problem, it can be difficult to direct resources to address that problem.
Efforts to raise the public’s awareness of racial/ethnic health care disparities have achieved modest success. In 2006, nearly 6 in 10 people surveyed believed African Americans received the same quality of care as Whites, and 5 in 10 believed Latinos received the same quality care as Whites (Figure 1).6 These estimates are similar to findings in the 1999 survey.7
Figure 1
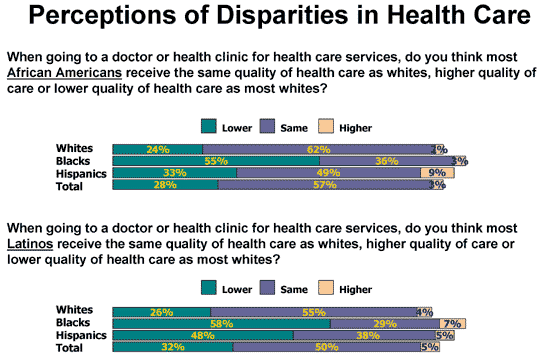
NOTE: Does not total 100% because ‘don’t know/refused’ not included. SOURCE: Kaiser Family Foundation, March/April 2006 Kaiser Health Poll Report Survey, April 2006 (Conducted April 2006).
In contrast to the general public’s continued lack of awareness, the level of awareness among physicians has risen sharply. In 2002, the vast majority (69%) of physicians said that the health care system “rarely or never” treated people unfairly based on an individual’s racial/ethnic background.8 In 2005, less than a quarter (24%) of physicians disagreed with the statement “minority patients generally receive lower quality care than White patients.”9
Expanding Health Coverage
Health insurance matters in determining whether and when people get necessary medical care, where they receive care, and how healthy people are. However, racial/ethnic minority populations – who constitute only about one-third of the U.S. population – are disproportionately represented among those without any health coverage (Figure 2). Compared with the insured, the uninsured are less likely to have a regular doctor or to get timely and routine care, and are more likely to be hospitalized for preventable conditions. Thus, expansions to health insurance coverage are of particular importance to racial/ethnic minority groups.
Figure 2
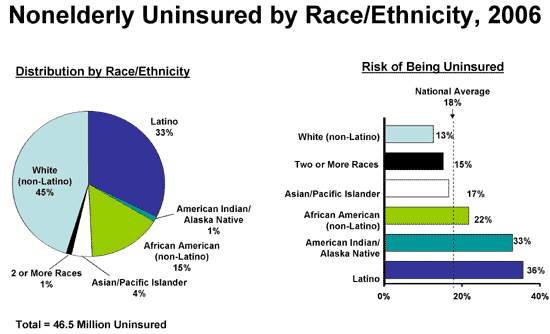
NOTE: American Indian group includes Aleutian Eskimos. SOURCE: Urban Institute and Kaiser Commission on Medicaid and the Uninsured analysis of the March 2007 Current Population Survey
Minority Americans are much less likely to have health insurance offered through their jobs, and even after accounting for work status, minority Americans are still more likely than Whites to be uninsured.10 As such, Medicaid, a source of coverage for many of the nation’s poor and disabled, is an important safety net for about 1 in 4 nonelderly African Americans, American Indians/Alaska Natives, and Latinos, and about 1 in 10 Asian/Pacific Americans and Whites.11
Efforts are needed to assure that existing sources of coverage, such as Medicaid, are maintained while also working to expand other sources of coverage for those who are uninsured.
Improving the Number and Capacity of Providers in Underserved Communities
Despite efforts since the 1970s to increase the number of health professionals in medically underserved areas, members of racial/ethnic minority groups are still underrepresented in the health care workforce and are more likely than Whites to live in neighborhoods that lack adequate health resources.12 For example, 28% of Latinos and 22% of African Americans report having little or no choice in where to seek care, while only 15% of Whites report this difficulty.13 African Americans and Latinos are also twice as likely as Whites to rely upon a hospital outpatient department as their regular source of care, rather than a doctor’s office where opportunities for continuity of care and patient-centered care are greater.14 This is a result of many factors, including the higher rates of uninsured and the limited availability of primary care physicians in some communities of color.
Even when health care resources are geographically accessible, language and cultural barriers are sometimes a problem.15 Approaches to strengthening communication and relationships between patients and providers include greater use of medical interpretation services, expanding the racial/ethnic diversity of the health professions workforce, and developing provider training programs and tools in cross-cultural education. Since minority health professional are more likely than Whites to practice in minority and medically underserved areas, a more diverse health workforce could help to improve access and adherence to treatment.16
Increasing the Knowledge Base
Although evidence of racial and ethnic health care disparities is substantial, the evidence-base for developing interventions to eliminate these disparities remains limited. For example, efforts are currently underway to examine how training health care providers to offer culturally and linguistically appropriate services, increasing the use of electronic medical records to decrease medical errors and improve coordination of care, and increasing the use of financial incentives to promote high quality health care may reduce racial and ethnic health disparities. In addition, there is a growing effort to address factors outside the health care system, such as socioeconomic status, education and geography, which have been shown to impact health status and access health care.17
Increasing the knowledge base will require investing in routinely collecting and analyzing data on health care use across racial/ethnic groups. Data from national surveys, health insurers, and different health settings are needed to better understand the problems and impact of interventions. One reason we know so little about patterns of health care use for many racial/ethnic groups is that we have not collected the data or have insufficient sample sizes in publicly available data sources. Yet, at a time when the heterogeneity of the population is increasing, funding for national surveys that measure disparities and track the nation’s progress in addressing them is being cut.
ASSESSING CANDIDATE POSITIONS
The Democratic and Republican presidential nominees have proposed broad health reform plans; however, addressing racial and ethnic health care disparities has not been a priority issue in the 2008 election. Senator John McCain seeks to control health care costs and expand coverage, but does not specifically address health disparities between racial and ethnic groups.18 Senator Barack Obama’s health plan would expand coverage to improve access, and explicitly states intentions to address the “root causes” of health disparities. The plan would require hospitals and health plans to collect, analyze and report health care quality data for disparity populations, increase diversity in the health workforce to ensure culturally competent care, and support and expand the capacity of safety-net institutions which disproportionately serve minority populations.19 Senator Obama also calls for the creation of a national HIV/AIDS strategy and would focus on eliminating disparities in communities hardest hit by the epidemic, many of which are communities of color.20
The following questions will help you evaluate the candidates’ proposals for addressing racial/ethnic health care disparities:
- What is the candidate’s general approach to reducing racial/ethnic disparities in health care?
- What is the candidate’s proposal to expand sources of insurance coverage? What would its impact be on minority groups?
- Does the candidate have a plan to increase prevention efforts for diseases that disproportionately impact communities of color?
- What is the candidate’s stance on diversity in the healthcare workforce?
- How does the candidate plan to hold government agencies accountable for monitoring and addressing racial/ ethnic disparities within the health care system?