 Blue Wall Voices Project
Report
Blue Wall Voices Project
Report
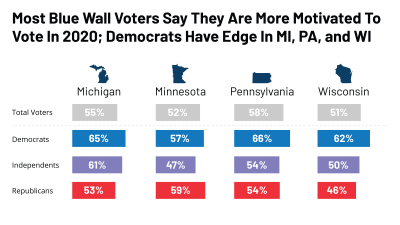
This partnership polling report from KFF and The Cook Political Report examining the attitudes and experiences of voters in in four states (Michigan, Minnesota, Pennsylvania, and Wisconsin) that were previously considered Democratic strongholds. It probes voters’ views of President Trump and the Democratic primaries, their motivations for voting, and issues including health care, the economy, immigration and trade a year out from the 2020 general election.