Talking About Medicare: Your Guide to Understanding the Program, 2012
Medicare Supplemental Insurance
![]() Download a printable pdf version of this section.
Download a printable pdf version of this section.
![]() Download a printable pdf version of the entire guide.
Download a printable pdf version of the entire guide.
- Basics of Medicare Supplemental Insurance (Medigap)
- Choosing a Medigap Policy
- Enrolling in a Medigap Plan
- Switching Medigap Policies
Medicare provides broad protection against the costs of many health care services, but has relatively high cost-sharing requirements and significant gaps in coverage. As a result, most beneficiaries have some form of supplemental coverage.
If you want to stay in Original Medicare, you may want to consider your options for supplemental coverage. Insurance that is supplemental to Medicare pays after Medicare. It helps pay Medicare costs and pay for care that Medicare does not, such as emergency care outside of the U.S. Without such coverage, your out-of-pocket costs could be high if you require medical care.
About one in three Medicare beneficiaries receive supplemental coverage through employer-sponsored retiree health coverage. If you have access to this type of supplemental coverage, there are advantages to keeping this coverage. Some retiree policies may be more generous than other types of coverage. They are sometimes less expensive than other policies, since employers tend to pay at least part of the cost. If you are not yet on Medicare, find out what employee benefits you may be eligible for when you go on Medicare, and ask how these benefits coordinate with Medicare.
Other beneficiaries who have limited incomes have access to supplemental coverage under Medicaid. Today, about 20 percent of Medicare beneficiaries are dually eligible for Medicare and Medicaid. For more information, see the Medicare and People with Low Incomes section.
For those in Original Medicare without access to employer-sponsored retiree health coverage or Medicaid, Medigap is one option for supplemental coverage. Medigap policies help make health care costs more predictable and stable. Medigap policies charge a monthly premium and cover some or all of your Medicare costs. Medigap policies typically require no additional paperwork to get your medical bills paid. Medicare usually pays its share of the health care bill and then sends it to your Medigap insurer to pay. Today, about one in five Medicare beneficiaries has supplemental insurance through an individually-purchased Medigap policy. The information below will address Medigap coverage, and will not discuss other sources of supplemental coverage.
Basics of Medicare Supplemental Insurance (Medigap)
If you want to buy a Medicare supplemental insurance policy, known as a “Medigap” policy, you will need to decide which benefit package to buy and which insurer to use. Before making a decision, it is helpful to understand what benefits are covered and how to compare plans.
There are 10 different standardized Medigap plans, labeled A, B, C, D, F, G, K, L, M, and N. Each Medigap plan pays for a particular set of benefits. Core benefits are benefits that every Medigap plan must cover, such as Medicare Part A copayments. Not all plans are available in all states. Massachusetts, Minnesota and Wisconsin have their own standardized Medigap plans.
Insurance companies that sell Medigap policies are not required to sell all Medigap plan types; however, they are required to offer at least plan A if they offer any other Medigap plans. Plan A offers the fewest benefits of the ten standardized Medigap plans.
The most popular Medigap plans are C and F; these two plan types are also the only two that cover both the Part A and Part B deductibles.
On June 1, 2010, plans M and N were created. Prior to June 1, 2010, there were also plans E, H, I, and J. While these plans are no longer sold, individuals who have these policies can keep their policy as it is, and will be able to continually renew it.
Plans sold starting June 1, 2010 will no longer include the at-home recovery benefit. All plans will now include hospice care as a core benefit.
Medigap plans K and L have high deductibles. This means that they only start paying in full for your care after you have spent a certain amount of money out-of-pocket. Compared to other Medigap options, these plans are designed to provide more protection when you are very sick but include less coverage of your initial expenses. They require you to pay part of your costs for most Medicare-covered services until you have spent a certain amount out of pocket each year. Once you reach your out-of-pocket limit, both plans cover all of your Medicare deductibles and coinsurance for that year. Medigap premiums often vary widely – even for identical plan coverage. The cost of your Medigap policy depends on the type of Medigap plan you choose, the company from which you buy your policy, and the cost of Medigap plans in the state or county where you live. Once you have chosen the plan you want, it pays to shop around. Plans with the same letter name offer the same benefits, but the premiums vary from company to company.
No Medigap insurance policy fills gaps in coverage for Medicare HMOs or any of the other Medicare Advantage private health plans. Should you select an HMO, PPO, or other type of Medicare Advantage plan, you should budget for any costs that the plan doesn’t cover.
For free assistance with understanding your options, contact your local State Health Insurance Assistance Program (see Additional Resources). More information about Medigap plans can be found at: www.medicare.gov/Publications/Pubs/pdf/02110.pdf.
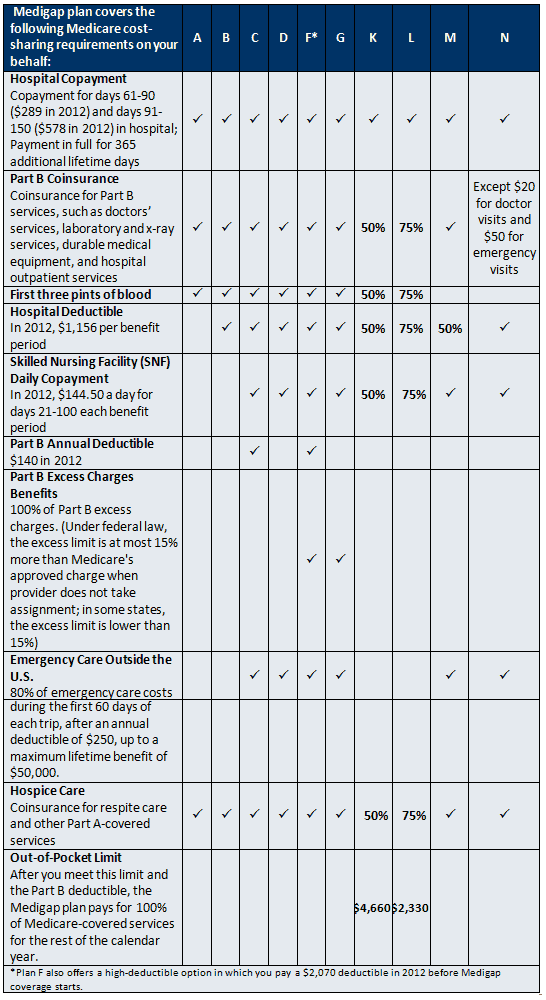
This chart shows the Medigap plan benefits for plans effective January 1, 2012:
Choosing a Medigap Policy
If you decide to purchase a Medigap policy, and have selected a type of plan (A-N), then the next step is to decide from which insurance company you wish to purchase your policy. The following steps will help you decide wisely.
- Call the insurance department in the state where you live for a list of companies that offer Medigap policies. Compare the premiums for the plan you want; premiums may vary considerably and rates may change each year.
- Understand how premiums are calculated and how they will change as you get older. Medigap premiums are calculated in three different ways:
- Attained-age rated: premiums are based on your current age, and typically increase as you get older. In states that allow this, if you keep your Medigap policy, your monthly premium might increase as you age.
- Issue-age rated: premiums are based on the age you are when you originally purchased the policy. Premiums are lower for people who purchase policies at a younger age. Once enrolled in a plan, your premiums won’t change based on your age, but they may go up because of inflation or other factors.
- Community-rated: premiums are the same for policyholders regardless of age; premiums may still increase because of inflation or other factors, but do not vary based on age.
After you’ve decided on the insurance company and Medigap plan that is best for you, contact the insurance company for a summary of the Medigap policy and an application. Fill out the application form carefully and completely. Remember, if you are applying for a policy in the first 6 months after you turn 65 and have Part B, or within 63 days of losing certain kinds of insurance, the insurance company cannot deny you a Medigap policy or change the price of a policy based on your answers to the medical questions. Your Medigap coverage typically begins on the first day of the month after you apply.
Enrolling in a Medigap Plan
You have the right to buy a Medigap policy only at certain times.
- Starting the month you turn 65 and are enrolled in Part B, you have an open enrollment period to sign up for any Medigap plan available in your state.
- If you are 65 or older, you have a “guaranteed issue right” to enroll in certain Medigap polices within 63 days of losing certain types of coverage, such as a retiree health plan or a Medicare Advantage plan.
These are the federal open enrollment periods. Some states have much broader open enrollment periods. Check with your state’s department of insurance for more information about enrollment rules in your state.
Federal law does not require Medigap insurers to sell Medigap policies to Medicare beneficiaries under age 65; however, some states do require insurers to sell Medigap policies to beneficiaries under age 65. If you are under 65, check with your state’s department of insurance or State Health Insurance Assistance Program for more information.
Under federal law, Medigap insurers cannot refuse to sell people age 65 or older a Medigap policy and cannot raise premiums because of a person’s health status during their open enrollment period or guaranteed issue period. Outside of these times, Medigap insurers can refuse to offer you a Medigap plan or can charge you higher premiums because of your health status, unless your state has more generous enrollment rules that prohibit them from doing so.
Additionally, if you are in a guaranteed issue period, your insurer cannot make you wait for coverage of pre-existing conditions. During your open enrollment period, plans can wait to cover your pre-existing conditions for up to six months unless you had continuous coverage from certain types of insurance for at least six months prior to enrolling in the Medigap plan.
Switching Medigap Policies
In most cases, insurance companies are not required to sell you a Medigap plan, unless you are in your 6-month open enrollment period or have guaranteed issue rights. As mentioned above, however, some states have more generous requirements. Check with your state’s insurance department about your Medigap rights and protections.
Before you switch to a new plan, be sure to compare the benefits and premiums before switching. As when you first purchased your Medigap policy, be sure to understand how your premiums are calculated, and how they may increase as you age.