Pulling it Together: Duals: The National Health Reform Experiment We Should Be talking More About
The Center for Medicare & Medicaid Services (CMS) and 26 states are moving to launch a large scale managed care demonstration project potentially involving millions of the poorest, sickest, most expensive Medicare and Medicaid beneficiaries, the so-called dual eligibles. The experiment is getting more and more attention from policy experts, but with controversial issues like the survival of the Affordable Care Act and converting Medicare to a premium support program grabbing the limelight, it has otherwise flown under the radar screen.
The 9.1 million dual eligible beneficiaries represent just a small share of the 97 million beneficiaries served by either Medicare or Medicaid but account for about 35 percent of all dollars spent by the two big programs. As a group they are sicker than other Medicare beneficiaries — half have three or more chronic conditions and six in ten have cognitive limitations, leading to increased use of health and long-term care services. While most are over age 65, four in ten are younger with permanent disabilities. Two of three are women. A striking 56 percent have incomes of less than $10,000 per year. (Kaiser.EDU, Medicare/Medicaid Dual Eligibles.)
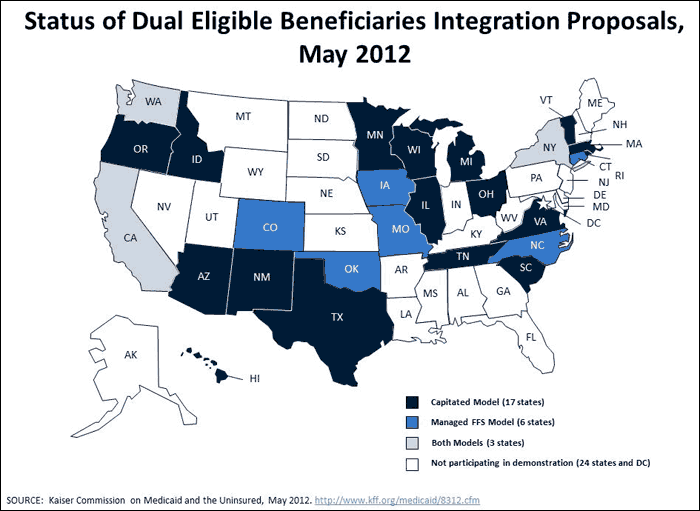
Of the 26 proposed state demonstrations, most are planning capitated managed care models, but some propose using a managed fee-for-service approach. For the capitated model, states and the federal government will enter a three-way contract with private managed care companies to manage the care of the enrolled population. Medicare, which mainly pays for acute care, and Medicaid, which mainly pays for long-term care, will blend payments into one rate, with savings taken off the top for both Medicare and Medicaid. The demonstration is moving quickly; half of the 26 states are looking to implement either the capitation or fee-for-service model in 2013 and others in 2014. Both the challenges and the potential of this health reform experiment are enormous. (Dx For A Careful Approach To Moving Dual Eligible Beneficiaries Into Managed Care Plans, Health Affairs, June 2012.)
Analysis by researchers on our staff and at the Urban Institute shows that while the duals as a group are higher utilizers than other Medicare beneficiaries, a smaller subset of duals are very high utilizers: 2 million of 9 million duals in 2007 (the last year for which merged Medicare and Medicaid data were available) were responsible for 60 percent of Medicare and Medicaid spending; the remaining 7 million duals accounted for 40 percent of spending (The Diversity of Dual Eligible Beneficiaries).
Some states will pursue broad demonstrations while others may pursue more targeted approaches, focusing on groups with recurring high expenses, such as nursing home residents. If states and health plans could target their efforts and more effectively coordinate the care of the very high utilizers, the benefits to both beneficiaries and the programs could be quite large.
In the capitated model, managed care companies will strike deals providing front-end savings to Medicare and Medicaid to manage the care of this population. The real challenge will be to assemble the delivery networks at the local level to effectively manage the broad range of services duals use, including behavioral health, pharmacy, community-based and institutional long-term care services, and a full range of acute care services. Managing care for a population that includes some who are very reliant on long term care, in particular, will require developing new networks of services for many managed care companies. So will managing care for a population with a high incidence of cognitive and mental health problems. Very few health plans now have the necessary experience to manage the care of this complex population and it will take time to develop new arrangements for appropriate services.
Medicaid is a federal-state program administered by the states and Medicare is a federal program, both with different populations and benefits (Medicare’s Role for Dual Eligible Beneficiaries; Medicaid’s Role for Dual Eligible Beneficiaries). It is predictable that there will be federal-state control issues to work through as a demonstration program involving a merger of both programs with private plans evolves. None of these challenges are reasons not to undertake the demonstration, only to recognize that implementation will take careful planning and time because the details of delivering care and services will matter.
I learned first-hand about the challenges of developing new service networks in the early days of Medicaid managed care in the 1980’s, as Human Services Commissioner in New Jersey. We established the first state-run, federally-qualified HMO for Medicaid. It achieved front-end savings and some ability to reallocate more of the Medicaid dollar to primary care. But we never were able to build the network of providers to more effectively manage care to improve outcomes or lower costs, for a population far less complex than the dual eligibles are.
Across the country Medicaid managed care slowly replaced fee for service for children and their parents but it never became the huge cost saver it was originally expected to be. Thirty years after it began to gain momentum Medicaid managed care is now moving to higher cost populations where the potential for savings are thought to be larger but the risks to sick patients are also greater.
With the spotlight on the ACA and Medicare and Medicaid budget challenges, this experiment involving millions of some of the highest cost, sickest people served by public programs has so far been under-reported. Eventually, covering this story will require getting inside delivery systems and interviewing policymakers, providers, and especially patients and their families, just the kind of journalism news organizations are hard pressed to do with their frayed budgets. This is not a breaking story a reporter can cover in one day. It will never have the drama of the highly politicized ACA and Medicare wars. But it deserves attention beyond our world of health policy.
Success in the dual eligibles demonstration could help reduce federal and state health spending in both big health care entitlement programs and improve the health of a very needy population. But the pressure to save money always cautions prudence, patience, and in this case careful targeting and customization of services, when large numbers of low-income people with disabilities and serious illnesses are involved.
